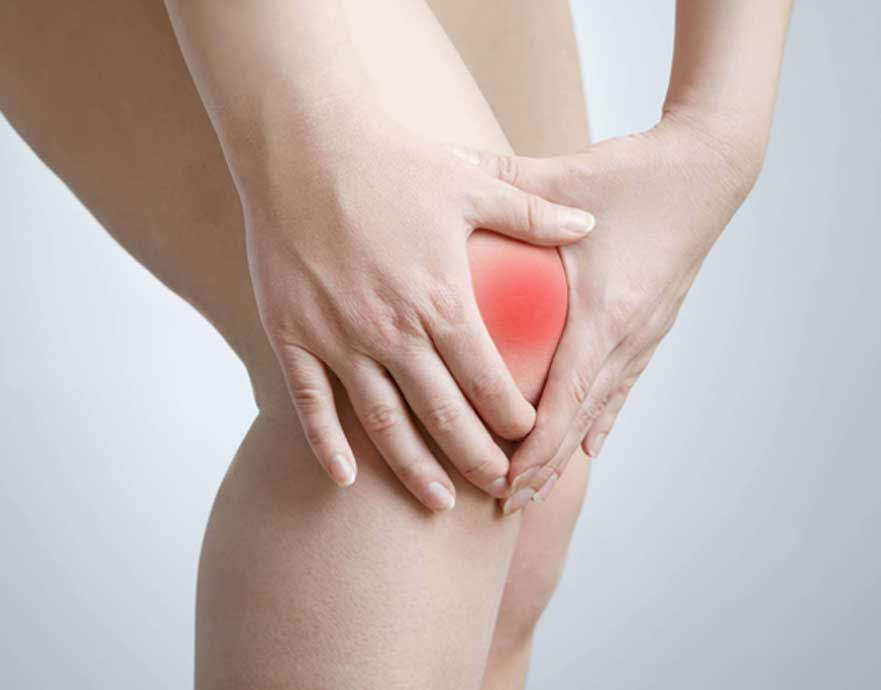
Learn more about Osteoarthritis and how LA Pain Associates can manage your symptoms.
The word “arthritis” actually applies to over 100 diseases affecting the joints. Osteoarthritis is the most common of these. Also known as degenerative arthritis or degenerative joint disease, it affects about 27 million people in the U.S. alone.
- While it can involve any joint, it is most common in the neck, lower back, hips, knees, fingers, and the bases of the big toe and thumb
- Most patients with osteoarthritis are over 65 years old
CONTACT US TODAY
Causes of Osteoarthritis
Normal joints have ends covered with a rubbery substance called cartilage that cushions the bones and enables the joints to move smoothly. In osteoarthritis, the cartilage starts to break down, so the joint does not move as smoothly and becomes swollen and painful. As the condition worsens, the patient may also develop bone spurs. The joint becomes inflamed, and that causes more damage to the cartilage. In advanced osteoarthritis, the cartilage wears away completely, so the bones rub against each other and cause more pain.
Osteoarthritis can be primary or secondary. Primary osteoarthritis occurs by itself and is not caused by a disease or injury; it is generally linked to the aging process. Secondary osteoarthritis, by contrast, is caused by another condition. Common causes of secondary osteoarthritis include repeated injury to a given joint, obesity, birth defects, gout, and diabetes.
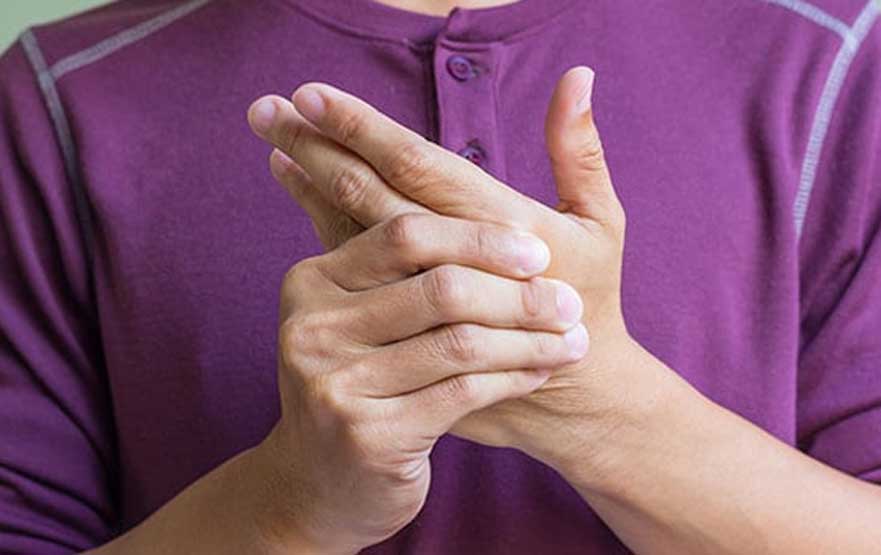
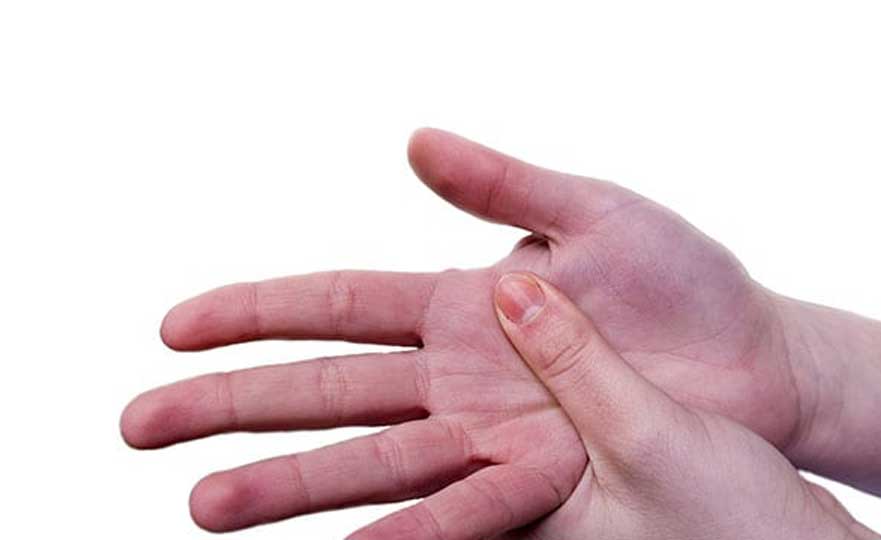
Symptoms
Osteoarthritis develops gradually, and the most common symptoms are pain and stiffness in the affected joint. The affected joint may also feel tender if someone presses on it. As the condition progresses, the patient will lose flexibility and range of motion in the affected joint. They may hear a grating sound when they try to use the joint as the bones scrape against each other. The patient may develop extra bits of bone called bone spurs around the affected joint; they will feel like hard lumps.
Diagnosing Osteoarthritis
The doctor will start by taking the patient’s medical history and conducting a physical exam. While there are no blood tests that can diagnose osteoarthritis, the doctor may order such tests if they believe the patient has secondary osteoarthritis and need to determine the cause.
The doctor may order X-rays to determine the location and severity of the joint damage. X-rays can also help the doctor find such problems as loss of cartilage, bone spurs and abnormally narrow spaces between bones of the affected joint. X-rays can also be used to rule out other possible causes of joint pain and decide if and when the patient needs surgery.
In joint fluid analysis, the doctor uses a needle to draw fluid from the arthritic joint. They will then perform tests to look for signs of inflammation or infection.
Treatments
Osteoarthritis is a chronic disease that currently has no cure. There are many treatments, however, and they aim to relieve pain and keep the patient as mobile as possible. Physical therapy will be an important part of any treatment program. Since obesity makes the osteoarthritis worse by increasing pressure on the joints, the patient will be encouraged to lose weight if necessary. Physical therapy will also help the patient increase their flexibility and range of motion. The doctor will prescribe various medications to relieve pain. In severe cases, they may recommend surgery to repair or even replace damaged joints.